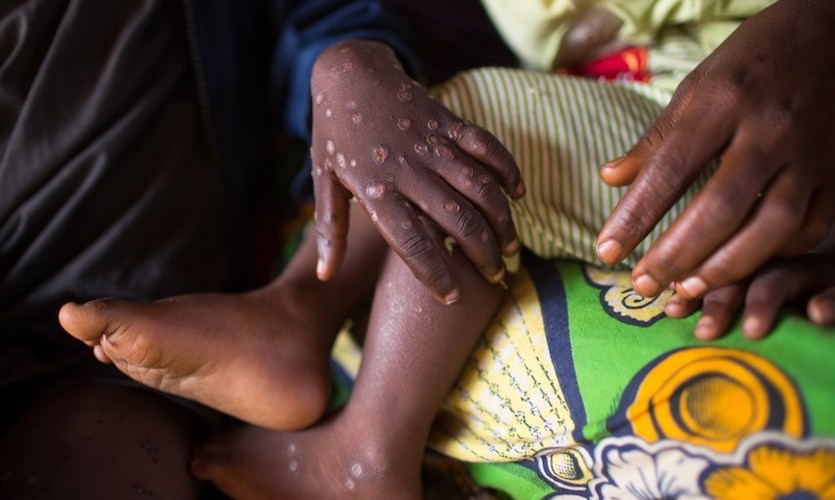
Monkeypox is a largely uncommon disease caused by infection from the monkeypox virus. The virus belongs to the genus ‘orthopoxvirus’ which is part of the ‘poxviridae’ family (a family of viruses).
Monkeypox was first identified in 1958, when outbreaks of a pox-like disease were detected in a colony of monkeys kept for scientific purposes in Denmark, after being transported from Malaysia. The first-ever human infection of the disease occurred in the Democratic Republic of the Congo in 1970, at the same time when intensive steps were being taken to control the Smallpox outbreak. Monkeypox has since been found in a number of central and western African nations apart from Congo, including Cameroon, Gabon, Liberia, Nigeria, and the Central African Republic. Cases of this disease observed in people living outside of the African continent have been connected to international travel and import of animals.
Symptoms
Monkeypox is classified as a viral ‘zoonotic’ disease by the World Health Organization (WHO), which means that it can be passed on to people through animals. The disease can also be spread through close human contact. According to WHO guidelines, symptoms of the condition include severe headaches, fever and chills, muscle and backache, poor energy levels, swollen lymph nodes, and skin rash. Rashes on the body can range from a few to several thousand in numbers, and can be slightly elevated or flat, possibly filled with highly infectious fluid. They are most commonly concentrated on the face, palms of the hands, and soles of the feet.
Treatment
In most cases, symptoms normally last between two to four weeks, subsiding on their own, without the need for treatment. However, medical complications and death are also probable in some individuals, particularly newborns and people with weakened immune systems. Therefore, it is advised that people seek medical attention immediately if they suspect they are suffering from symptoms similar to those of monkeypox.
There is no specific vaccine against Monkeypox, but there are various vaccines available for Smallpox immunity that provide a certain degree of protection against monkeypox as well. Original smallpox vaccines are no longer available to the general population due to a halt in production, in 1980. A newer vaccine called ‘Imvamune’ was developed and authorised for Smallpox in 2019, although it is not widely available yet. Nonetheless, the WHO is working with the manufacturer to improve access to the vaccination.
Outbreak
Ever since Britain confirmed the first case of Monkeypox on May 7, 2022, the WHO has reported approximately 400 suspected or confirmed cases till date, from countries that are not endemic to the disease. The UN body’s leading Monkeypox expert Rosamund Lewis had earlier suggested that there is no need to panic over the virus. When asked if there is a chance of another global pandemic, she acknowledged that it is unlikely that Monkeypox will turn into one since it is possible to put an end to the outbreak before it gets any larger.
Read more: From COVID To Ukraine: How Do We Explain It To Children?
What About India?
So far, no cases of Monkeypox have been reported in India. Even so, the Ministry of Health has already developed regulations for dealing with a potential outbreak. Several standards have been proposed to ensure that all healthcare institutions across the country are prepared to deal with an unlikely crisis situation. The ministry has made it clear that even a single case recorded will amount to the disease being labelled as an outbreak.
The Indian Council of Medical Research (ICMR) and the National Centre for Disease Control have been instructed to keep a close check on the situation. Airports have been directed to be on the lookout for any sick passengers who have returned from a Monkeypox-affected country and isolate them. All states and union territories have been directed to quickly report any suspicious case to the state and Centre’s surveillance units. According to the guidelines, a confirmed case is supposed to be monitored daily, for 21 days, to keep an eye on the symptoms. Furthermore, the guidelines emphasise the necessity of raising public awareness about the disease, practising basic hygiene, and utilising a Personal Protective Equipment (PPE) kit when treating patients.